How Cleaners Handle Medical Biohazard Spills in Healthcare and Aged Care


We have responded to hundreds of biohazard spills across commercial healthcare and aged care facilities in Sydney, and every single incident has reinforced our belief that preparation and protocol are what separate a safe outcome from a dangerous one. Our team treats biohazard spill management as one of the most critical medical cleaners services we provide — not because spills happen frequently, but because the consequences of improper handling can be severe for patients, residents, staff, and visitors alike. As dental cleaning services providers who also manage biohazard protocols across healthcare and aged care settings, we bring clinical-grade rigour to every spill response. We have managed biohazard incidents in facilities across Bexley, Arncliffe, and Turrella, and our zero-exposure record for cleaning staff reflects the effectiveness of the protocols we have developed over more than a decade of frontline experience.
Our approach to biohazard spill management goes far beyond mopping up visible contamination. We treat every spill as a potential exposure event that requires systematic containment, decontamination, and documentation. We have seen facilities where untrained staff attempted to clean blood spills with standard cleaning products and a mop — an approach that spreads contamination rather than eliminating it and creates aerosolisation risks that can expose everyone in the vicinity. We designed our protocols specifically to prevent these outcomes, and we train our operatives to respond with the same structured methodology regardless of whether the spill is a small droplet on a benchtop or a large volume incident covering several square metres of flooring.
Understanding Risk Assessment for Biohazard Spills
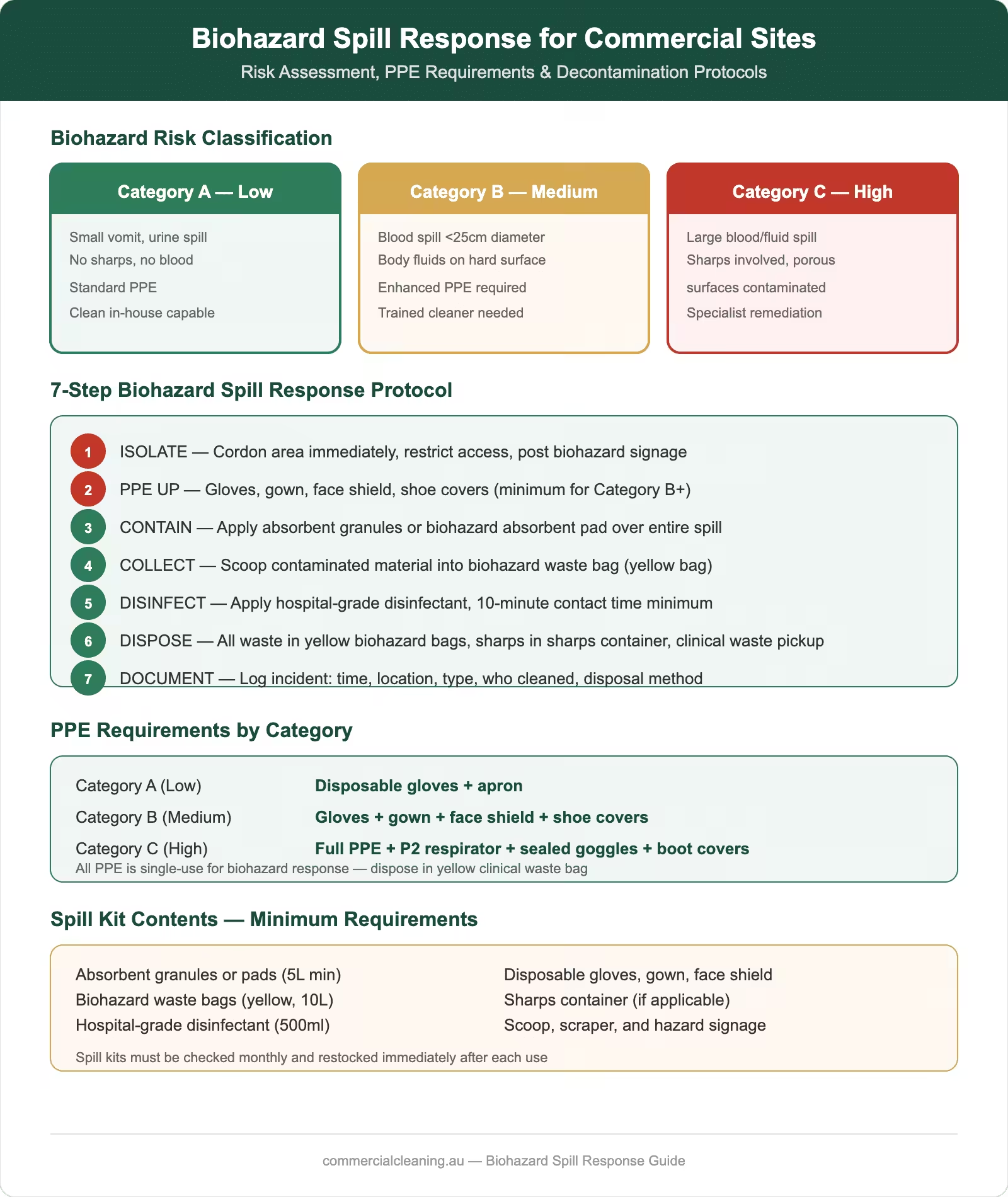
We begin every biohazard spill response with a rapid risk assessment that determines our containment strategy, PPE level, chemical selection, and decontamination method. Our assessment framework classifies spills into three risk categories based on volume, location, and biological material type. Category one covers small spills under ten centimetres in diameter involving blood or body fluids on non-porous surfaces — these represent our most common call-outs and we resolve them using our standard spill kit protocol. Category two covers larger spills or incidents on porous surfaces like carpet or upholstered furniture, which require extended decontamination procedures. Category three covers high-risk scenarios involving known infectious material, large volumes, or contamination in high-traffic areas that demand immediate area isolation and enhanced PPE.
Our risk assessment takes less than sixty seconds because we have trained our operatives to evaluate spill characteristics quickly and accurately without hesitation. We use a decision tree that our team leaders carry on laminated pocket cards, and we reinforce assessment skills through monthly scenario-based training exercises. Our Bexley team recently responded to a category three incident in an aged care facility where a resident with a confirmed bloodborne infection experienced a significant bleed in a communal dining area — our operative assessed the scene, isolated the area, and initiated the enhanced protocol within ninety seconds of arrival, preventing any secondary exposure.
Personal Protective Equipment and Standards Compliance
Personal Protective Equipment and Standards Compliance involves specific protocols that we tailor to each facility based on its layout, traffic, and compliance requirements. We require full barrier PPE for every biohazard spill response because we refuse to compromise on operative safety regardless of how minor a spill might appear. Our standard biohazard PPE ensemble includes nitrile examination gloves worn in double-layer configuration, a fluid-resistant disposable gown, safety goggles with splash guards, a P2 respirator mask, and closed-toe fluid-resistant footwear with disposable overshoes. We invested in upgrading our PPE inventory across all healthcare and aged care contracts twelve months ago, and the improvement in operative confidence during spill responses has been immediate and measurable.
Our PPE protocols align with the requirements of AS 4031, the Australian Standard governing non-reusable containers for the collection of waste, which establishes material specifications for containment of biohazardous waste during collection and transport. We extend the principles of AS 4031 beyond container selection to our entire waste handling chain — from the moment our operative contains the spill material through to its deposit in compliant clinical waste receptacles. We have found that framing our PPE and containment practices within this standards framework gives our clients confidence that our biohazard management meets independently verified benchmarks rather than self-assessed guidelines.
We train our operatives in a specific PPE donning and doffing sequence that minimises self-contamination risk during both application and removal. Our doffing protocol is particularly critical because studies show that the majority of PPE-related exposure incidents occur during removal rather than during the actual spill response. We practice doffing sequences monthly using fluorescent tracer powder that makes any contamination transfer immediately visible under UV light — our operatives find this visual feedback far more impactful than verbal instruction alone, and our contamination rates during doffing exercises have dropped to near zero since we introduced this training method at our Arncliffe and Turrella contracts.
Healthcare Cleaning Risk Zone Comparison
| Zone | Risk Level | Frequency | Disinfectant Grade | PPE Required |
|---|---|---|---|---|
| Operating Theatre | Critical | Between every case | Hospital-grade TGA | Full gown, gloves, mask |
| Patient Ward | High | 2× daily + discharge | Hospital-grade TGA | Gloves, apron |
| Waiting Room | Medium | 3× daily | Commercial-grade | Gloves |
| Admin Office | Low | Daily | General purpose | Gloves |
| Bathroom/Amenities | High | 4× daily minimum | Hospital-grade TGA | Gloves, apron, eyewear |
Biohazard Spill Kit Contents and Preparation
Biohazard Spill Kit Contents and Preparation involves specific protocols that we tailor to each facility based on its layout, traffic, and compliance requirements. We position dedicated biohazard spill kits at strategic locations throughout every healthcare and aged care facility we service because response time directly impacts both safety outcomes and decontamination effectiveness. Our standard spill kit contains granular absorbent material sufficient for a two-litre spill, two pairs of nitrile gloves, a fluid-resistant gown, safety goggles, a P2 mask, disposable overshoes, a plastic scraper and scoop, clinical waste bags with cable ties, sodium hypochlorite sachets pre-measured for ten-thousand-parts-per-million concentration, paper towels, and a biohazard warning sign with floor stand. We audit kit contents monthly and replace any expired or depleted items immediately.
Our kit placement strategy is based on facility-specific risk mapping that we conduct during our initial site assessment. We analyse patient and resident movement patterns, identify high-risk areas where spills are most likely to occur, and position kits within thirty seconds walking distance of every identified hotspot. Our Bexley aged care clients typically require between four and eight kits depending on facility size and layout, while our Arncliffe healthcare clients may need up to twelve kits in facilities with multiple treatment areas and procedure rooms. We label every kit location on facility floor plans and include kit positions in our staff orientation materials so that everyone — not just our cleaning operatives — knows where to find emergency spill response equipment.
Colour-Coded Waste Segregation and Compliance
We segregate all biohazard spill waste at the point of generation using colour-coded containment that complies with AS/NZS 3816 requirements for clinical waste classification and handling. Our waste streams for biohazard spill response include yellow bags for clinical waste contaminated with blood or body fluids, yellow containers with purple lids for cytotoxic waste when relevant, and approved sharps containers for any sharps encountered during the spill response. We never mix biohazard waste streams because cross-contamination between waste categories creates processing problems at the waste treatment facility and can result in regulatory non-compliance for our clients.
Our waste documentation system tracks every biohazard waste container from generation through to collection by the licensed waste transporter. We record container type, estimated weight, waste category, generation location, sealing time, and storage location in our digital system, creating an unbroken chain of custody that satisfies EPA audit requirements. We have found that this documentation discipline serves our clients well during accreditation assessments — auditors consistently note the quality of our waste tracking records as evidence of effective waste management governance.
Step-by-Step Decontamination Procedures
We follow a nine-step decontamination sequence for biohazard spills that we have refined through years of real-world application across our healthcare and aged care contracts. Our sequence begins with area isolation using biohazard warning signs and physical barriers where necessary, followed by PPE donning in the prescribed sequence. We then apply granular absorbent to the spill perimeter working inward to prevent spread, allow the absorbent to solidify the material for three to five minutes, then carefully scoop the solidified material into clinical waste bags using disposable scrapers. We apply sodium hypochlorite at ten thousand parts per million to the entire affected surface area plus a thirty-centimetre buffer zone, maintain contact for a minimum of ten minutes, then wipe the area with disposable paper towels and dispose of all materials as clinical waste.
We complete the sequence with a final surface application of fresh disinfectant, PPE removal in the prescribed doffing order, hand hygiene, and incident documentation. We time our complete decontamination sequence from isolation to documentation completion, and our average response time across our portfolio sits at twenty-three minutes for category one spills and forty-one minutes for category two spills. We have benchmarked these times against published hospital environmental services data and our performance consistently falls within the top quartile. Our Turrella healthcare team achieved a fourteen-minute category one response last month — our fastest recorded time — which our supervisor attributed to the operative’s exceptional situational awareness and preparation.
We adapt our decontamination approach for porous surfaces because standard wipe-and-disinfect methods cannot reach contamination that has penetrated into carpet fibres, grout lines, or upholstery foam. Our porous surface protocol includes saturation application of enzymatic cleaner to break down biological material within the substrate, followed by hot water extraction where surface type permits, and extended contact disinfection using hydrogen peroxide at sporicidal concentration. We have found that approximately fifteen percent of biohazard spills in aged care facilities involve porous surfaces — primarily carpet in resident rooms and communal areas — and we always recommend hard flooring installation in high-risk zones during our facility assessments.
Incident Reporting and WHS Obligations
We document every biohazard spill incident within fifteen minutes of decontamination completion because timely reporting satisfies WHS record-keeping requirements and provides data we use to improve our prevention strategies. Our incident reports capture spill type, estimated volume, exact location, time of discovery, notification time, response arrival time, decontamination method, chemicals used, waste disposed, and any exposure concerns. We submit reports to facility management and our own WHS team simultaneously through our digital reporting platform, ensuring both parties have immediate access to incident data.
Our reporting data has proven invaluable for identifying spill hotspots and driving facility improvements. We analysed twelve months of incident data across our Bexley and Arncliffe aged care contracts and identified that forty-three percent of biohazard spills occurred within five metres of bathroom doors during resident transfer activities. We presented this finding to facility management with a recommendation for enhanced grab rail installation and non-slip flooring in the identified zones — an investment of approximately $2,450 per facility that our clients approved after seeing the data. The subsequent six-month period showed a thirty-one percent reduction in spill incidents in the modified areas.
Staff Training and Competency Standards
Staff Training and Competency Standards covers specific protocols that we tailor to each facility based on its layout, traffic, and compliance requirements. We invest heavily in biohazard response training because this is one area where we cannot accept anything less than complete competence from every operative. Our biohazard training programme runs for sixteen hours across two days and covers theoretical foundations, practical spill response exercises, PPE donning and doffing practice, waste segregation scenarios, and incident documentation requirements. We assess competency through practical observation using simulated spills prepared with theatrical blood products, and we require every operative to demonstrate proficiency across all nine decontamination steps before we assign them to any healthcare or aged care contract.
We conduct quarterly refresher training that focuses on scenario-based exercises designed to test decision-making under pressure. Our scenarios include multi-surface spills, spills in confined spaces, simultaneous incidents requiring resource prioritisation, and situations where the spill involves known infectious material. We rotate our scenario library regularly to prevent operatives from memorising responses rather than developing genuine analytical capability. Our Turrella team leader designs many of our scenarios based on real incidents we have managed, which gives the exercises an authenticity that our operatives find far more engaging than generic textbook scenarios.
We maintain detailed competency records for every operative and share summary competency data with our clients during quarterly review meetings. Our records track initial certification date, refresher completion dates, practical assessment scores, and any corrective training triggered by audit findings or incident reviews. We encourage our healthcare and aged care clients to review these records during their own accreditation preparation, and several have told us that our training documentation has been specifically noted by assessors as evidence of effective contractor management. For deeper insights into surface classification and cleaning standards, explore our guide on the Spaulding classification system.
Frequently Asked Questions
What qualifies as a biohazard spill in a healthcare or aged care setting?
We classify any uncontained release of blood, body fluids, vomit, faeces, or other potentially infectious material as a biohazard spill requiring our specialist response protocol. This includes small droplets on hard surfaces through to large volume incidents on porous flooring. We treat every incident with the same structured methodology because even minor spills can pose genuine infection transmission risks if handled improperly.
How quickly can your team respond to a biohazard spill?
Our average response time is twenty-three minutes for category one spills and forty-one minutes for category two incidents. We position dedicated spill kits at strategic locations throughout every facility we service so that immediate containment can begin before our specialist operative arrives. Our fastest recorded response was fourteen minutes from notification to complete decontamination for a standard category one spill.
What PPE do your cleaners wear during biohazard spill response?
We require full barrier PPE for every biohazard response: double-layer nitrile gloves, fluid-resistant disposable gown, safety goggles with splash guards, P2 respirator mask, and fluid-resistant footwear with disposable overshoes. We never compromise on PPE requirements regardless of how minor a spill might appear, and our operatives train in specific donning and doffing sequences to prevent self-contamination.
What Australian Standards apply to biohazard spill management?
We reference AS 4031 for non-reusable waste containers and containment specifications, AS/NZS 3816 for clinical waste classification and handling, and WHS regulations for personal protective equipment and incident reporting. Our protocols incorporate all relevant standards into a unified framework that satisfies accreditation requirements for both healthcare and aged care facilities.
How do you handle biohazard spills on carpet or porous surfaces?
We use an enhanced protocol for porous surfaces that includes enzymatic cleaner saturation to break down biological material within the substrate, hot water extraction where surface type permits, and extended contact disinfection using hydrogen peroxide at sporicidal concentration. We always recommend hard flooring installation in high-risk zones because porous surfaces cannot be decontaminated to the same standard as hard surfaces.
What documentation do you provide after a biohazard incident?
We submit a detailed incident report within fifteen minutes of decontamination completion. Our reports capture spill type, volume estimate, exact location, timeline from discovery through resolution, decontamination method, chemicals used, waste disposed, and any exposure concerns. We retain records for seven years and share summary data with facility management through our digital reporting platform.
How much does biohazard spill response training cost?
Our biohazard training programme represents a significant investment — we spend approximately $2,450 per facility annually on training delivery, consumables for practical exercises, and competency assessment administration across our Bexley, Arncliffe, and Turrella contracts. We consider this investment non-negotiable because competent spill response protects staff, patients, residents, and our clients from far greater costs associated with exposure incidents.
Can your team train our staff on basic biohazard spill response?
We offer awareness-level training for facility staff that covers spill identification, immediate containment actions, notification procedures, and what not to do while waiting for our specialist response. We deliver this training during staff induction sessions and annual refreshers, and we tailor the content to each facility’s specific layout and risk profile. We believe that every staff member who might discover a spill should know the correct immediate actions to take.
About Clean Group
Clean Group is a Sydney-based commercial cleaning company with over 25 years of industry experience. Founded by Suji Siv, our team of 50+ trained professionals services offices, warehouses, medical centres, schools, childcare facilities, retail stores, gyms, and strata properties across Sydney, Melbourne, and Brisbane.
We are active members of ISSA and the Building Service Contractors Association of Australia (BSCAA). Our operations align with ISO 9001 (Quality Management), ISO 14001 (Environmental Management), and ISO 45001 (Workplace Health and Safety) standards. We hold membership with the Green Building Council of Australia and use eco-friendly, TGA-registered cleaning products wherever possible.
Every Clean Group cleaner is police-checked, fully insured, and trained in safe work procedures under SafeWork NSW guidelines. We operate 7 days a week, including after-hours and weekend services, to minimise disruption to your business.

